Secretory Immunoglobin A (SIgA)
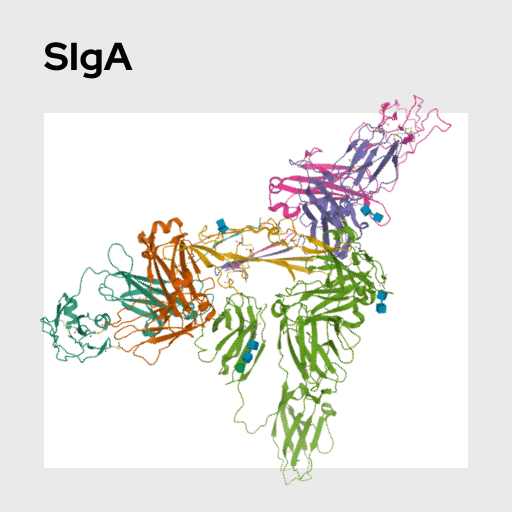
Secretory Immunoglobin A (SIgA) is the most common antibody found in mucosal membranes where it acts as a first line of defense against pathogens that invade bodily secretions. Like other antibodies, SIgA is produced and released by B cells. Levels of SIgA are often used as measure of mucosal immune activation in response to psychosocial stress.
Name: Secretory Immunoglobin A (IgA)
Category: Health and inflammation
Type of test: Saliva
Secretory Immunoglobulin A (IgA/SIgA) is an antibody that is found within the body’s mucosal membranes. MA greater amount of IgA is produced in the mucosal membranes than all other forms of antibodies combined. Because the body’s mucosal membranes are exposed to a more open environment than the inside of the body, IgA plays a key role in frontline immune defenses. IgA that is found in mucosal tissues exists primarily in a dimeric structure (pIgA), but further modification is needed to allow for stable excretion through the epithelium. With the addition of a J chain, the dimeric IgA-J chain complex becomes nearly stable enough for secretion. This synthesis is performed by submucosal B lymphocytes, at which point the final step is completed by the epithelial cells themselves. A ‘secretory component’ functions as a receptor for the pIgA, which then allows the secretory IgA (SIgA) to undergo transcytosis towards the apical membrane and, eventually, exocytosis into the mucosal environment. Without binding the secretory component, the IgA would be degraded by proteases present in these areas, so this step is critical in ensuring IgA functions properly.
Unlike many antibodies such as IgM, IgA does not efficiently activate the complement system. It can, however, prevent pathogenic entry into epithelial tissue by binding to the portions of the pathogen that it uses to translocate into the body. Additionally, because it does not have a high degree of binding specificity, it is able to recognize a broad variety of microorganism structures and can adhere to molecules that pathogens use to form colony structures. IgA has also been shown to sterically hinder interaction of pathogens with epithelial cells, further limiting any interaction that could result in infection
IgA has been implicated in numerous pathologies including, but not limited to, celiac disease, HSP, IgA nephropathy, and genetic conditions such as selective IgA deficiency. Levels of sIgA also tend to increase in the context of acute stress. Numerous bacteria are capable of secreting proteases that target and destroy IgA, and in recent years IgA has been implicated in chronic diseases such as Alzheimer's disease, with low IgA being observed in severe and moderate AD subjects. As the role of our own immune system in chronic disease becomes increasingly relevant, so too do questions about the role that specific immune components such as IgA might play in the etiology of these conditions.
Campos-Rodríguez, R., Godínez-Victoria, M., Abarca-Rojano, E., Pacheco-Yepez, J., Reyna-Garfias, H., Barbosa-Cabrera, R. E., & Drago-Serrano, M. E. (2013). Stress modulates intestinal secretory immunoglobulin A. Frontiers in Integrative Neuroscience, 7, 86. https://pubmed.ncbi.nlm.nih.gov/24348350/
Corthésy, B. (2013). Multi-Faceted Functions of Secretory IgA at Mucosal Surfaces. Frontiers in Immunology, 4, e00185. (link)